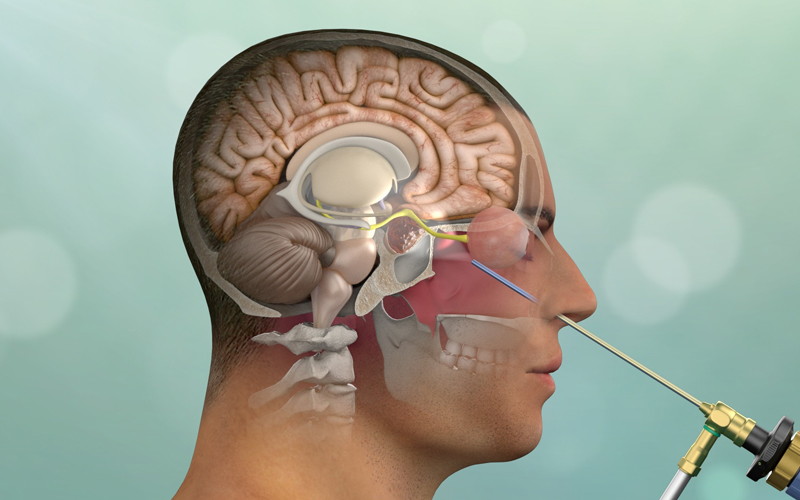
Endoscopic Brain Surgery
Endoscopic Brain Surgery is a minimally invasive neurosurgical technique that uses a thin, flexible tube with a camera and light at its tip — called an endoscope — to access and treat brain conditions. This advanced approach allows the neurosurgeon to operate through small incisions or natural openings (like the nostrils), reducing trauma to healthy brain tissues.
Endoscopic surgery is especially useful for treating certain tumours, cysts, and conditions involving the ventricles (fluid-filled cavities in the brain) or the skull base. The procedure offers greater precision, fewer complications, faster recovery, and better cosmetic outcomes compared to traditional open surgery.
Conditions Treated with Endoscopic Brain Surgery
Our centre specializes in endoscopic techniques for a variety of brain and skull base conditions, including:
-
Pituitary Adenomas: Tumours affecting hormones and often causing vision problems.
-
Craniopharyngiomas: Benign growths near the pituitary gland.
-
Colloid Cysts: Cysts blocking cerebrospinal fluid pathways in the brain.
-
Intraventricular Tumours: Tumours located within the brain’s ventricles.
-
Hydrocephalus: Abnormal fluid accumulation, often treated with Endoscopic Third Ventriculostomy (ETV).
-
Rathke’s Cleft Cysts & Other Sellar/Suprasellar Lesions.
-
Skull Base Tumours: Such as chordomas and meningiomas.
-
Selected Brain Cysts or Benign Lesions.
Advantages of Endoscopic Brain Surgery
Endoscopic surgery provides several key benefits for patients:
-
Minimally Invasive: Smaller incisions or natural access routes mean less trauma.
-
Reduced Blood Loss: Smaller operative fields minimize bleeding.
-
Lower Risk of Complications: Decreased risk of infection and damage to surrounding tissues.
-
Faster Recovery: Shorter hospital stay and quicker return to normal activities.
-
Less Pain and Scarring: Often requires no visible external incision.
-
Improved Visualization: High-definition cameras provide clear, magnified views of deep-seated areas.
How the Procedure Works
1. Preoperative Planning
-
Detailed MRI and CT scans help map the tumour or lesion.
-
Endoscopic approach is chosen based on the location and size of the lesion.
-
Patients are counseled about the procedure, benefits, and recovery.
2. The Surgery
-
Performed under general anesthesia.
-
A small incision or natural opening (such as through the nostrils in endonasal surgery) is used.
-
The endoscope, equipped with a high-definition camera, guides the surgeon.
-
Microsurgical or specially designed instruments are used alongside the endoscope to remove the tumour or treat the lesion.
-
In some cases, neuronavigation and intraoperative neuro-monitoring (IONM) are used to improve safety and precision.
3. Postoperative Care
-
Patients are closely monitored in the recovery area or ICU for a short period.
-
Most patients experience less pain and quicker recovery compared to traditional open surgeries.
-
Follow-up scans are performed to ensure complete removal and to monitor healing.
Recovery & Follow-Up
-
Hospital stays are generally shorter (2–4 days).
-
Most patients return to normal daily activities within a few weeks.
-
Regular follow-up visits and imaging help monitor for recurrence or complications.
-
For pituitary surgeries, hormone levels are checked and managed by the medical team.
Why Choose Us for Endoscopic Brain Surgery
-
Experienced Neurosurgeon & Neuro-Oncosurgeon: Skilled in advanced endoscopic techniques for both brain and skull base tumours.
-
State-of-the-Art Technology: High-definition endoscopic systems, neuronavigation, and intraoperative imaging for precision.
-
Multidisciplinary Team: Collaboration between neurosurgeons, ENT specialists (for endonasal surgeries), endocrinologists, and rehabilitation experts.
-
Minimally Invasive Expertise: Focused on achieving maximum safety with minimal disruption to healthy tissues.
-
Comprehensive Care: From preoperative counselling to rehabilitation, we provide complete support for optimal recovery.
When to Seek Medical Advice
Consult a specialist if you or your loved one experience:
-
Persistent or worsening headaches.
-
Visual disturbances, such as double vision or loss of peripheral vision.
-
Hormonal imbalances, unexplained weight changes, or fatigue.
-
Symptoms of hydrocephalus, like headaches, nausea, or difficulty walking.
-
A diagnosed brain tumour or skull base lesion suitable for a minimally invasive approach.
Early evaluation and timely intervention improve treatment outcomes and help preserve vital neurological functions.